Thalassemia Signs, Symptoms, Causes & Treatments
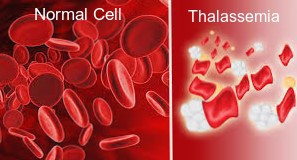
Thalassemia is a genetically inherited blood disorder characterized by abnormal hemoglobin production. It can be mild, moderate to severe resulting in lower hemoglobin, and may cause mild to severe anaemia. Hemoglobin is the protein molecule in red blood cells that carries oxygen. If you have mild thalassemia, you may not need treatment; thalassemia Signs, Symptoms depend upon the severity. But if you have a more severe form of the disorder, you may need regular blood transfusions. It is most common among people of Italian, Greek, Middle Eastern, South Asian, and African descent.
Thalassemia Signs, and symptoms:
The signs and symptoms depend on the type and severity of your condition.
- Weakness & Fatigue
- Pale or yellowish skin
- Bone deformities, especially in the Skull & face. It makes bone marrow expanded, bones thin and brittle, increasing the risk of broken bones.
- Dark urine
- Enlarged spleen
- Delayed growth and development
- Short of breath
- Heart problems: Congestive heart failure and abnormal heart rhythms may be associated with severe thalassemia.
- People with thalassemia may have an increased risk of infection.
Cause:
Thalassemia is caused by an abnormality or mutations in the gene of cells that make hemoglobin. It is genetic inherited blood disorder is passed from parents to children. Thalassemia disrupts the normal production of hemoglobin and healthy red blood cells, causing anemia.
If only one of the parents is a carrier of thalassemia, you may develop a form of the disease known as thalassemia minor. If this occurs, you probably won’t have Signs, or symptoms; but you will be a carrier of the disease. Some people with thalassemia minor may develop mild symptoms. If both of your parents are carriers of thalassemia, you have a greater chance of inheriting a more serious form of the disease.
How can thalassemia affect pregnancy?
Women with thalassemia may encounter fertility difficulties. If you have thalassemia, or if you carry a thalassemia gene, consider talking with a genetic counsellor for guidance if you’re thinking of having children.
Pregnancy carries the following risk factors in women with thalassemia:
- High risk of infection
- Hypothyroidism
- Gestational diabetes
- Heart problems
- Low bone density
Types of thalassemia:
There are two main types of thalassemia, alpha(α) thalassemia and beta(β) thalassemia. The thalassemia is classified according to which chain of the haemoglobin molecule is affected. In alpha -thalassemia, production of the alpha globin chain is affected, while in beta-thalassemia, production of the beta globin chain is affected.
Alpha (α) Thalassemia:
Four genes, 2 from each parent, are required to make alpha globin protein chains. When 1 or more genes are missing, it produces alpha thalassemia. The severity of thalassemia depends on how many genes are faulty.
- One faulty gene: The patient has no symptoms. A healthy person who has a child with symptoms of thalassemia is a carrier. This type is known as alpha thalassemia minima.
- Two faulty genes: The patient has mild anaemia. It is known as alpha thalassemia minor.
- Three faulty genes: The patient has haemoglobin H disease, a type of chronic anaemia.
- Four faulty genes: Alpha thalassemia major is the most severe form of alpha thalassemia. It is known to cause Hydrops fetalis with Hemoglobin Barts, a serious condition in which fluid accumulates in parts of the fetus’ body.
Beta (β) Thalassemia:
We need two globin genes to make beta-globin chains, one from each parent. If one or both genes are faulty, beta thalassemia will occur. beta – thalassemia growth problems, bone abnormalities such as osteoporosis, and an enlarged spleen (the organ in the abdomen that plays a part in fighting infection). Severity depends on how many genes are mutated.
- One faulty gene: This is called beta thalassemia minor, patients may be relatively asymptomatic.
- Two faulty genes: There may be moderate or severe symptoms. This is known as thalassemia major, it may be intermedia. β thalassemia major is called Colley’s anaemia.
Diagnosis:
Thalassemia can be diagnosed via a complete blood count, haemoglobin electrophoresis, and DNA testing. Perform DNA analysis to diagnose thalassemia or to determine if a person is carrying mutated haemoglobin genes.
Treatments:
Treatments will be depending upon your condition. Get check-up regularly by your doctor for proper treatments & follow your doctors’ advice.
- With a mild case, you may not need treatment.
- If it is serious, you might have to get regular blood transfusions. How often you need blood transfusions can vary.
- Regular blood transfusions they can cause too much iron in the blood. That can lead to problems with the heart, liver, and blood sugar. If you get transfusions, you and your doctor will talk about whether you need medicine that can help remove extra iron from your body. Sometimes, transfusions of blood cause high fever, chills, nausea, diarrhoea and low blood pressure.
- In some condition bone marrow transplant, remove the spleen or gallbladder may be needed.
- Follow your doctor advice & eat a healthy diet.
- The doctor may advise supplements like calcium and vitamin D.
- Don’t take iron pills.


0 Comments